TSW - Topical Steroid Withdrawal ICD-10: L27.1
Often searched as: red skin syndrome, steroid withdrawal skin, topical steroid addiction, skin burning after stopping steroid cream, eczema cream dependency, skin worse after stopping hydrocortisone, TSW symptoms, red burning skin steroid rebound…
Clinical urgency level
Systems Affected
Severity Levels
mild
Localized rebound redness and itching in the area where topical steroids were stopped, limited to the original treatment site, manageable with moisturizers and cold compresses. Symptoms resolve within weeks.
moderate
Redness, burning, and skin sensitivity spreading beyond the original treatment area. Significant oozing, peeling, or papulopustular rash. Sleep disruption and daily functioning affected. May last 3–12 months. Requires supportive care and possible specialist evaluation.
severe
Widespread (full-body or near-total) red, burning, oozing, and peeling skin. Severe pain, debilitating fatigue, thermoregulatory dysfunction (inability to control body temperature), intense insomnia, hair loss, and complete inability to work or function. May last 1–3+ years. Requires urgent specialist evaluation, multidisciplinary support, and possible systemic therapy (dupilumab, cyclosporine).
Red Flags
- Spreading redness, burning, or oozing that goes far beyond the original eczema or skin condition area after stopping topical steroids
- Intense burning pain (not just itching) — burning is the hallmark symptom that distinguishes TSW from eczema
- Thermoregulation failure: sweating abnormally or being unable to regulate body temperature
- Skin cycling through cycles of redness → oozing → tight dry skin → peeling → repeat, in waves
- Severe insomnia from burning pain
- Elephant-like skin thickening or severe atrophy in areas of long-term steroid use
- Systemic symptoms: lymph node swelling, flu-like malaise, intense fatigue
- Progressive worsening — not improving — after stopping steroids despite proper skincare
- Eyelid swelling and facial skin involvement with burning (classic 'red sleeve' pattern on arms)
- History of long-term topical steroid use followed by rebound worse than original condition
Clinical Presentation
Stage 1. Inflammation - TSW

Source: TSW Assist (tswassist.com)
Stage 2. Exudation, Oozing and Scab Formation

Source: TSW Assist (tswassist.com)
Stage 3. Proliferation and Flaking

Source: TSW Assist (tswassist.com)
Stage 4. Remodelling
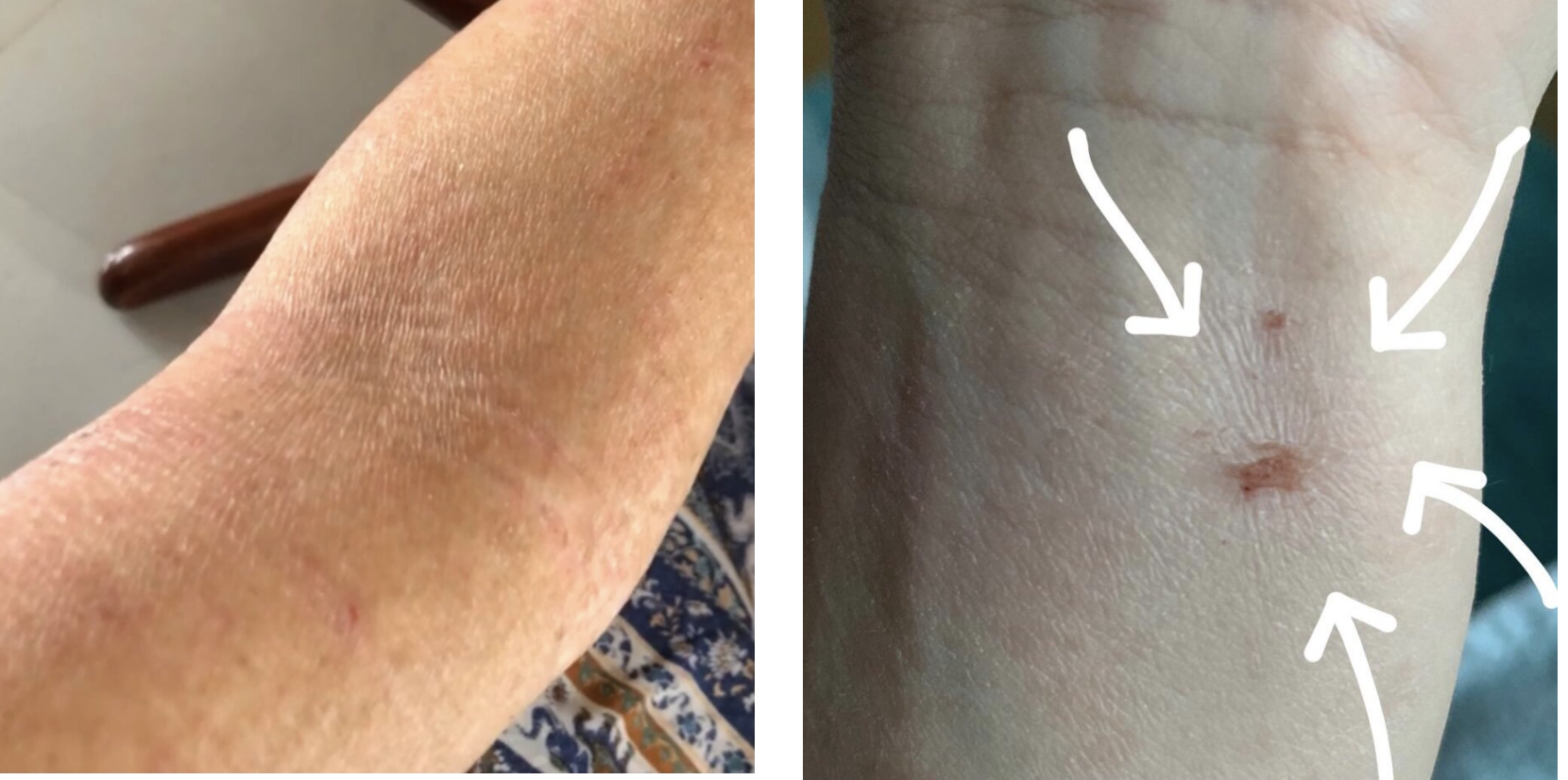
Source: TSW Assist (tswassist.com)
When to See a Doctor
Seek medical evaluation if you have been using topical corticosteroids regularly for more than 3 months and notice your skin is becoming increasingly red, reactive, or dependent — requiring stronger steroids to control symptoms that were previously controlled by weaker ones. This is steroid addiction. If you have stopped steroids and are experiencing widespread burning, oozing, and spreading redness beyond your original skin condition, see a dermatologist experienced in TSW immediately. If you are considering stopping long-term topical steroids, do NOT stop abruptly without medical supervision — discuss a tapering strategy or transition to non-steroidal treatments (tacrolimus, dupilumab) with your doctor first.
Differential Diagnosis
- Atopic dermatitis / eczema flare (most common misdiagnosis — key distinction: TSW causes burning not primarily itching, spreads beyond original sites, and does NOT respond to more steroids; eczema responds to steroids)
- Contact dermatitis (allergic or irritant — patch testing to identify allergen)
- Erythroderma from other causes (psoriasis, cutaneous T-cell lymphoma, drug reaction — biopsy may be needed)
- Seborrheic dermatitis (facial redness — responds to antifungals)
- Rosacea (central facial redness — no oozing, history of steroid use distinguishes)
- Perioral dermatitis (perioral papulopustular — often caused by topical steroids on the face)
- Cutaneous T-cell lymphoma (rare — patch stage mimics eczema; biopsy needed in atypical cases)
- Psoriasis (well-defined silvery plaques — biopsy if uncertain)
Comorbidities
- Atopic dermatitis (the most common underlying condition for which steroids were originally prescribed — TSW and AD can coexist, making diagnosis complex)
- Contact dermatitis (may have led to long-term steroid use)
- Perioral dermatitis (frequently caused by facial topical steroid use)
- Skin atrophy and striae (from long-term TCS use — may persist after TSW resolves)
- HPA axis suppression (hypothalamic-pituitary-adrenal — with prolonged potent TCS use, especially in children)
- Secondary bacterial infections (Staphylococcus aureus superinfection of open, weeping skin)
- Severe depression, anxiety, and PTSD (from prolonged debilitating skin condition with little medical recognition)
- Social isolation and inability to work during active TSW
Prognosis
TSW is a self-limiting condition — the skin does eventually recover completely without permanent damage in the majority of cases, but the timeline is highly variable and often prolonged. Mild TSW may resolve within 1–3 months. Moderate cases typically last 6–12 months. Severe or long-duration cases can last 2–4 years or longer, with fluctuating cycles of improvement and relapse. There is no evidence-based treatment that significantly accelerates recovery, though dupilumab (anti-IL-4/IL-13 biologic, approved for atopic dermatitis) has shown benefit in patients with concurrent AD and TSW. Cyclosporine may reduce severity in some. Moisturizers, wet wraps, cold compresses, antihistamines for itch, and pain management support quality of life during recovery. The prognosis for full skin recovery is good — but the psychological and social burden during TSW can be severe. Community support (ITSAN — International Topical Steroid Awareness Network) has been critical for patients who are often dismissed or misdiagnosed.
Detailed Overview
Tags

Analyze your skin and hair with AI
Instantly analyze your skin with AI and get personal recommendations.
- - Get instant skin analysis
- - Personalized results from AI

* The scan result is not a diagnosis. To obtain a diagnosis and a treatment recommendation, consult your doctor.
Explore more conditions
Learn about other skin and hair conditions.